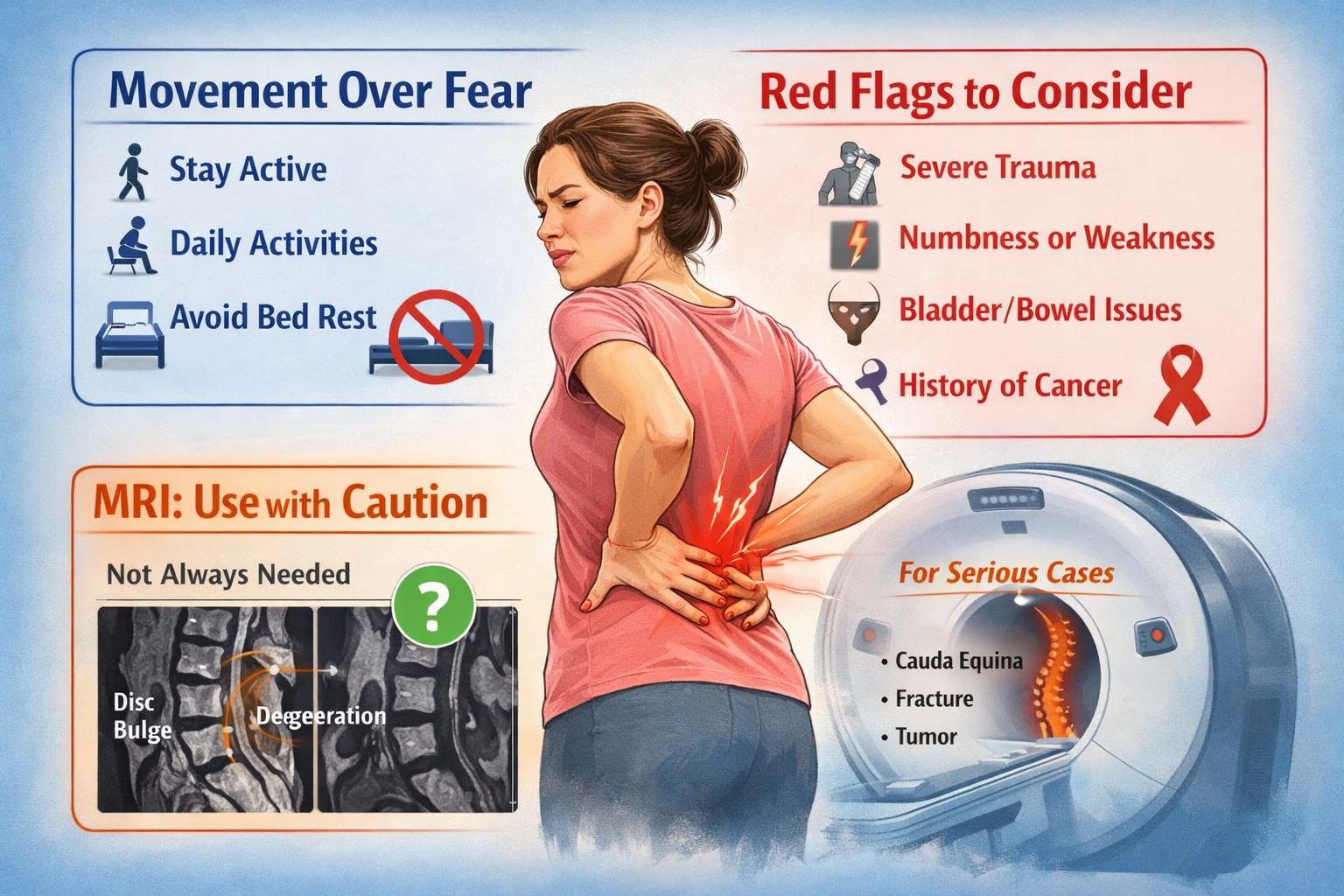
Most episodes of low back pain are not a sign that something dangerous is falling apart. In the first few weeks, the goal is usually not to hunt for a dramatic MRI finding, but to sort out the rare serious cases, preserve function, and avoid making pain more frightening than it already is.
Back pain escalates into a disaster story very quickly. A few painful days, and people start looking for a “slipped disc,” a “trapped nerve,” or the first sign of permanent damage. Then comes an MRI, followed by a report full of bulges, degeneration, protrusions, and a new layer of anxiety. The problem is that this script often causes more trouble than the pain itself. For most adults with an acute episode of non-specific low back pain, the overall prognosis is favorable: pain and disability usually improve substantially in the first six weeks, even though symptoms do not always disappear immediately and recurrences are common.
That does not mean back pain should be brushed off. It means common should not be mistaken for catastrophic. Major guidelines are broadly aligned on the essentials: first rule out serious pathology and major neurologic deficit; if those are absent, avoid routine imaging, support self-management, and encourage people to stay as active as they reasonably can. NICE recommends advice tailored to the patient, including encouragement to continue normal activities, and says imaging should be considered only if the result is likely to change management. The VA/DoD guideline similarly includes “advice to remain active” in self-care and emphasizes early assessment for serious causes.
What usually helps in the first few weeks
The least glamorous recommendation is often the most useful: do not default to bed rest. Evidence summarized in Cochrane reviews found that advice to stay active offers small benefits, or at minimum is not worse, compared with advice to rest in bed for acute low back pain. That fits neatly with current guideline practice: keep moving within tolerance, keep doing ordinary tasks, and avoid dropping out of daily life altogether. In practice, that usually means walking, changing positions, pacing activity, and avoiding the trap of waiting for perfect comfort before moving again.
Medication is not the centerpiece, but it can have a role. The American College of Physicians guideline lists nonpharmacologic care first for acute and subacute low back pain, and if medication is needed, it supports NSAIDs or skeletal muscle relaxants as options. What matters here is not the fantasy of a drug that fixes the episode, but the more modest aim of symptom control while people stay functional.
Exercise is where public advice often gets ahead of the evidence. People are routinely told that the right routine will quickly “fix” an acute episode, but the evidence for exercise therapy in acute non-specific low back pain is not especially strong. By contrast, the evidence is more supportive in chronic low back pain, where a Cochrane review found moderate-certainty evidence that exercise probably helps pain, although functional gains are smaller. That distinction matters: movement is usually helpful early on, but it is not the same as claiming that a special corrective program reliably solves acute pain.
Paracetamol is a good example of why habit should not be confused with evidence. It was long treated as an almost automatic first step, but the PACE trial found that regular or as-needed paracetamol did not improve recovery time compared with placebo in acute low back pain.
Why early MRI often does not help
MRI has a powerful reputation. It feels like the test that should finally reveal what is wrong. But in non-specific low back pain without red flags, routine early imaging does not improve clinical outcomes. Chou’s systematic review and meta-analysis found that immediate routine lumbar imaging did not improve pain, function, or other outcomes in patients without signs of serious underlying disease. That is why NICE recommends imaging only when it is likely to change management, and why the ACR rates initial imaging as usually not appropriate for acute low back pain with or without radiculopathy when there are no red flags.
There is another problem: MRI is extremely good at finding abnormalities that are also common in people with no pain at all. Brinjikji and colleagues showed that degenerative spinal imaging findings are common in asymptomatic people and become more common with age; many of these findings are likely part of normal aging rather than a clear pain generator. In other words, a report can be technically true and clinically misleading at the same time.
That is why early MRI often changes the story more than the prognosis. It can pull the conversation away from function, time course, and risk assessment, and toward anatomical language that sounds ominous but may not explain the symptoms at all. Used well, imaging is a decision-making tool. Used badly, it can become a reassurance ritual that adds noise.
Red flags: what really matters, and what is often overstated
Red flags matter, but they do not work as cleanly as popular medical content suggests. In a large primary care cohort, serious pathology was found in only 0.9% of patients with acute low back pain, while at least one red flag was present in 80.4%. The practical lesson is simple: a single red flag is not a diagnosis, and it is not an automatic MRI referral. It is a clue that should raise or lower suspicion in the context of the whole clinical picture.
Some situations do deserve a much higher index of suspicion. For possible cauda equina syndrome, the VA/DoD guideline highlights urinary retention, urinary or fecal incontinence, saddle anesthesia, and changes in rectal tone. Those symptoms justify urgent evaluation, typically including urgent MRI. At the same time, the evidence on diagnostic accuracy is sobering: a systematic review found that classic red flags for cauda equina syndrome have poor sensitivity, so the absence of a textbook presentation does not reliably exclude it.
For fracture, the strongest red flags are not random scary descriptors but a fairly recognizable set: older age, severe trauma, prolonged corticosteroid use, and, even more importantly, combinations of red flags. For malignancy, a prior history of cancer is the single most useful red flag in the evidence. Many widely repeated warnings, such as night pain by itself or age alone, are much weaker than they are often made to sound.
The broader point is that red flags should support clinical reasoning, not replace it. The international framework on red flags for serious spinal pathologies was developed precisely because serious causes are rare, but missing them matters; the framework is meant to guide assessment, not turn every checkbox into a diagnosis.
When imaging is actually useful
Saying that MRI is often unnecessary is not the same as saying it is unhelpful. Imaging becomes useful when it answers a real clinical question. In practice, that usually means one of four scenarios: there is a serious or progressive neurologic deficit; there is suspicion of cauda equina syndrome, infection, fracture, or cancer; symptoms are persistent or worsening to the point that invasive treatment is being considered; or the result is genuinely likely to change management in specialist care. NICE, VA/DoD, and ACR all frame imaging in essentially those terms.
That distinction matters. MRI is most useful as a tool for decisions, not as a tool for panic reduction. When treatment choices actually depend on the scan, imaging is timely and valuable. When they do not, the scan often adds more interpretation problems than solutions.
Why avoiding catastrophizing matters
“Do not catastrophize” does not mean “it is all in your head.” It means the language around pain has consequences. Systematic reviews show that catastrophizing is associated with poorer outcomes in people with low back pain, and modern guidelines increasingly recognize the role of psychosocial factors in shaping recovery. The VA/DoD guideline explicitly recommends considering psychosocial factors, and tools such as STarT Back or Örebro are part of that broader risk-stratified mindset.
A good explanation is part of treatment. No one should promise that nothing serious is going on before a proper assessment. But there is also no need to turn every episode of back pain into a story about a damaged spine. A better frame is this: first make sure there are no signs of a serious cause, then preserve movement and function, manage symptoms sensibly, and watch the trajectory before rushing to anatomical explanations. That is a better match for both the prognosis and the evidence.
Bottom line
Most people with a new episode of low back pain do not need dramatization. They need risk sorting, a clear explanation, some time, and a plan that helps them stay functional. Evidence-based care is fairly consistent here: rule out serious causes, avoid overusing imaging, encourage ordinary activity, and do not mistake alarming MRI language for a diagnosis. That is not minimization. It is a more accurate and more useful way to care for back pain.
Sources
- NICE. Low back pain and sciatica in over 16s: assessment and management (NG59).
- VA/DoD. Clinical Practice Guideline for the Diagnosis and Treatment of Low Back Pain. 2022.
- American College of Radiology. ACR Appropriateness Criteria: Low Back Pain.
- Costa LCM, et al. The prognosis of acute and persistent low-back pain: a meta-analysis. CMAJ. 2012.
- Chou R, et al. Imaging strategies for low-back pain: systematic review and meta-analysis. Lancet. 2009.
- Brinjikji W, et al. Systematic Literature Review of Imaging Features of Spinal Degeneration in Asymptomatic Populations. AJNR. 2015.
- Henschke N, et al. Prevalence of and screening for serious spinal pathology in patients presenting to primary care settings with acute low back pain. Arthritis Rheum. 2009.
- Downie A, et al. Red flags to screen for malignancy and fracture in patients with low back pain: systematic review. BMJ. 2013.
- Dionne N, et al. What is the diagnostic accuracy of red flags related to cauda equina syndrome, when compared to MRI? A systematic review. Musculoskelet Sci Pract. 2019.
- Dahm KT, et al. Advice to rest in bed versus advice to stay active for acute low-back pain and sciatica. Cochrane Database Syst Rev. 2010.
- Williams CM, et al. Efficacy of paracetamol for acute low-back pain: a double-blind, randomised controlled trial. Lancet. 2014.
- Hayden JA, et al. Exercise therapy for chronic low back pain. Cochrane Database Syst Rev. 2021.
- Wertli MM, et al. Catastrophizing as a prognostic factor for outcome in patients with low back pain: a systematic review.
- Finucane LM, et al. International Framework for Red Flags for Potential Serious Spinal Pathologies. JOSPT. 2020.
- WHO. Guideline for non-surgical management of chronic primary low back pain in adults in primary and community care settings. 2023.